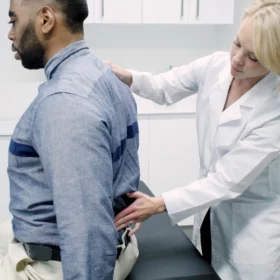
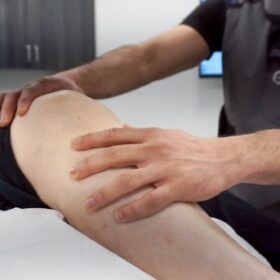
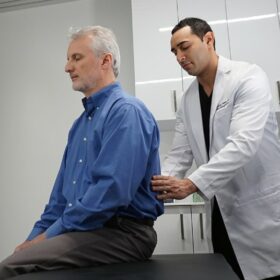
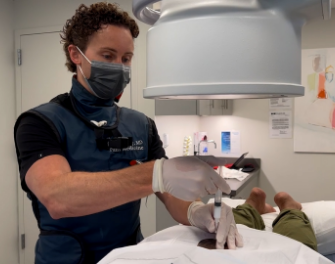
Building a Strong Partnership with Your Pain Doctor
At Pain Treatment Specialists, we understand that managing chronic pain involves forming a solid partnership between you and your pain doctor. We believe in a collaborative approach that empowers you to take an active role in your treatment. In this article, we explore key strategies for fostering a strong partnership with your pain doctor, ensuring you receive the comprehensive care and support you deserve.
Are you interested in get more information about your condition or get a treatment?
Fill the form below to start!
1. Communicate Openly
Communication is crucial in any successful partnership, and the relationship with your pain doctor is no exception. Establishing open lines of communication from the outset sets the stage for trust and understanding. Don’t hesitate to express your concerns, questions, or preferences regarding your pain management plan. Whether it’s during appointments, via phone calls, or through messaging platforms, we encourage you to communicate openly with us.
Questions to Ask Your Pain Doctor:
- What is the underlying cause of my pain, and what diagnostic tests or evaluations are needed to confirm the diagnosis?
- What are the potential treatment options available for my condition, and what are the risks and benefits associated with each approach?
- Can you explain the expected outcome of the recommended treatment plan, including the timeline for improvement and any potential side effects?
- Are there any lifestyle modifications or complementary therapies that could enhance the effectiveness of my treatment?
- How frequently should I schedule follow-up appointments to monitor progress and adjust the treatment plan if necessary?
- What steps can I take to minimize the risk of medication dependence or misuse while managing my pain?
- Are there any clinical trials or emerging therapies that may be appropriate for my condition?
- Can you provide recommendations for additional resources or support services to help me cope with the emotional and psychological aspects of chronic pain?
- How can I communicate with you outside of scheduled appointments if I have questions or concerns about my treatment?
- What is your approach to managing pain flare-ups or unexpected changes in symptoms, and what steps should I take in such situations?
2. Be Prepared
Time with your pain doctor is precious, so it’s essential to come prepared for each appointment. Before your visit, jot down any symptoms you’ve experienced, changes in your pain level, and any questions or topics you want to discuss. Bringing along a list of current medications, including dosages and any supplements you’re taking, can also streamline the conversation and ensure nothing is overlooked. By actively participating in the appointment process, you’ll maximize the value of each interaction and contribute to informed decision-making.
Tips to Prepare for Your Appointment:
- Write down your current symptoms, including any changes in pain intensity or location, and note any triggers or exacerbating factors.
- Compile a comprehensive list of all medications you’re currently taking, including prescription medications, over-the-counter drugs, vitamins, and supplements, along with their dosages.
- Jot down any questions or concerns you want to discuss with your pain doctor during the appointment.
- Bring along any relevant medical records, imaging reports, or previous treatment documentation to provide context for your current condition.
- Consider keeping a pain diary leading up to the appointment, recording details such as pain levels, activities, and medication use to help your pain doctor better understand your pain patterns and treatment response.
- Arrive at your appointment a few minutes early to complete any necessary paperwork and ensure a smooth check-in process.
- Wear comfortable clothing that allows easy access to the area(s) of pain for physical examination or assessment.
- Bring a trusted friend or family member with you to the appointment for support, assistance in taking notes, and to provide additional insights into your pain experience if needed.
- Prepare to actively participate in the discussion about your treatment plan, including asking questions, expressing preferences, and collaborating with your pain doctor.
- Consider using a notebook, smartphone, or voice recorder to capture important information shared during the appointment for future reference.
3. Educate Yourself
Empowerment begins with education. Take the initiative to learn about your specific condition, available treatment options, and potential side effects. Reliable resources, such as reputable medical websites, peer-reviewed journals, and materials provided by Pain Treatment Specialists, can equip you with the knowledge needed to make informed decisions about your care. When you understand the rationale behind your treatment plan, you become an active participant in the process, driving better outcomes and enhancing your overall experience.
4. Set Realistic Goals
Setting realistic goals is essential for tracking progress and maintaining motivation throughout pain management. Collaborate with your pain doctor to establish measurable objectives that align with your treatment priorities and lifestyle. Whether it’s improving functionality, reducing pain intensity, or enhancing quality of life, clearly defined goals serve as a roadmap for guiding treatment decisions and evaluating efficacy. Remember that progress may occur gradually, so celebrate small victories along the way and adjust your goals as needed.
5. Embrace a Multidisciplinary Approach
Chronic pain is complex and multifaceted, often requiring a multidisciplinary approach for optimal management. At Pain Treatment Specialists, we advocate for a holistic approach that addresses not only the physical aspects of pain but also its emotional, psychological, and social dimensions. Depending on your individual needs, your pain management plan may incorporate a combination of interventions, such as physical therapy, minimally invasive pain treatments, and lifestyle modifications. By embracing a comprehensive approach to care, we can tailor solutions that target the root causes of your pain and promote long-term well-being.
Multidisciplinary, Minimally Invasive Treatments Offered at PTS:
- RICE (Rest, Ice, Compression, Elevation): RICE is a simple yet effective approach for managing acute injuries or flare-ups of chronic pain. It involves resting the affected area, applying ice to reduce inflammation, using compression to support the injured area, and elevating the limb to minimize swelling. RICE helps alleviate pain and promotes healing by reducing inflammation and providing support to the injured tissues.
- Physical Therapy: Physical therapy focuses on restoring function, mobility, and strength through tailored exercise programs, manual therapy techniques, and education. By addressing muscle imbalances, improving flexibility, and enhancing body mechanics, physical therapy helps alleviate pain, improve function, and prevent future injuries.
- Epidural Steroid Injections: Epidural steroid injections deliver a combination of corticosteroid medication and local anesthetic directly into the epidural space surrounding the spinal cord and nerve roots. This targeted approach reduces inflammation and pain associated with conditions such as herniated discs, spinal stenosis, and radiculopathy by suppressing nerve irritation and decreasing swelling.
- Facet Joint Injections: Facet joint injections involve injecting a combination of local anesthetic and corticosteroid medication into the small joints located along the spine. These injections help alleviate pain and inflammation caused by facet joint arthritis, injury, or mechanical stress by numbing the affected nerves and reducing inflammation within the joint.
- Trigger Point Injections: Trigger point injections target specific areas of muscle tightness or knots, known as trigger points, with a mixture of local anesthetic and corticosteroid medication. By inactivating trigger points and releasing muscle tension, these injections help alleviate pain and improve range of motion in conditions such as myofascial pain syndrome and muscle spasms.
- Viscosupplementation: Viscosupplementation involves injecting a thick fluid called hyaluronic acid into the knee joint to lubricate and cushion the joint surfaces. This minimally invasive treatment is used to alleviate pain and improve mobility in patients with osteoarthritis by restoring the natural viscosity and shock-absorbing properties of the synovial fluid.
- Nerve Blocks: Nerve blocks involve injecting a local anesthetic or medication directly into a specific nerve or group of nerves to interrupt pain signals and provide temporary pain relief. These injections can target various nerves throughout the body, including peripheral nerves, sympathetic nerves, and spinal nerves, to alleviate pain associated with conditions such as neuropathy, complex regional pain syndrome (CRPS), and trigeminal neuralgia.
- Radiofrequency Ablation: Radiofrequency ablation (RFA) is a minimally invasive procedure that uses heat generated by radiofrequency energy to disrupt the function of nerves responsible for transmitting pain signals. By creating a lesion along the targeted nerve pathway, RFA interrupts pain transmission and provides long-lasting pain relief for conditions such as facet joint arthritis, sacroiliac joint dysfunction, and chronic neck or back pain.
- Spinal Cord Stimulation: Spinal cord stimulation (SCS) involves implanting a small device, similar to a pacemaker, near the spinal cord to deliver mild electrical impulses to the nerves. These impulses interfere with pain signals traveling to the brain, effectively reducing pain perception and providing relief for chronic pain conditions such as failed back surgery syndrome, neuropathy, and complex regional pain syndrome (CRPS).
6. Foster Mutual Respect
Mutual respect forms the bedrock of any successful partnership. Recognize that you and your pain doctor bring unique expertise to the table, each contributing valuable insights and perspectives. While you’re the expert on your own body and lived experience, your pain doctor offers specialized medical knowledge. By fostering mutual respect and collaboration, we can work together as equal partners in pursuit of your health and wellness.
7. Prioritize Self-Care
Amidst the challenges of chronic pain, it’s crucial not to overlook the importance of self-care. Incorporate self-care practices into your daily routine, such as mindfulness meditation, gentle exercise, adequate sleep, and healthy nutrition. Engage in activities that bring you joy and fulfillment, whether it’s spending time with loved ones, pursuing hobbies, or immersing yourself in nature. By prioritizing self-care, you empower yourself to better cope with pain.
Self-Care Tips to Manage Chronic Pain:
- Practice Mindfulness and Relaxation Techniques: Engage in mindfulness meditation, deep breathing exercises, or progressive muscle relaxation to promote relaxation, reduce stress, and alleviate muscle tension associated with chronic pain.
- Maintain a Healthy Lifestyle: Follow a balanced diet rich in fruits, vegetables, lean proteins, and whole grains to support overall health and well-being. Stay hydrated, limit caffeine and alcohol intake, and avoid smoking to minimize inflammation and optimize pain management.
- Stay Active Within Your Limits: Incorporate regular low-impact exercises such as walking, swimming, cycling, or gentle stretching into your routine to improve flexibility, strengthen muscles, and enhance mood. Listen to your body and adjust activities based on your pain levels to prevent exacerbating symptoms.
- Prioritize Quality Sleep: Establish a consistent sleep schedule, create a relaxing bedtime routine, and create a comfortable sleep environment conducive to restorative sleep. Practice good sleep hygiene habits, such as avoiding screens before bedtime and limiting stimulating activities, to improve sleep quality and reduce pain sensitivity.
- Manage Stress: Identify stressors in your life and develop coping strategies to manage stress more effectively. Techniques such as journaling, spending time in nature, engaging in hobbies, or seeking support from loved ones can help reduce stress levels and alleviate pain.
- Utilize Heat and Cold Therapy: Apply heat packs, warm baths, or heating pads to sore or tense muscles to increase blood flow, relax muscles, and alleviate pain. Alternatively, use cold packs or ice packs to numb painful areas, reduce inflammation, and numb pain receptors.
- Practice Good Posture and Body Mechanics: Maintain proper posture and body mechanics during daily activities to minimize strain on muscles and joints. Use ergonomic furniture, adjust workstations to optimize alignment, and take regular breaks to stretch and rest to prevent muscle imbalances and reduce pain.
- Engage in Enjoyable Activities: Make time for activities that bring you joy and fulfillment, whether it’s spending time with loved ones, pursuing hobbies, or enjoying nature. Engaging in enjoyable activities can distract from pain, boost mood, and improve overall well-being.
Consult Our Board-Certified Interventional Pain Specialists at PTS
Pain Treatment Specialists is dedicated to providing compassionate care and building strong relationships with our patients. Led by board-certified interventional pain doctors, we specialize in offering minimally invasive treatments that prioritize your well-being.
At PTS, we take a holistic approach to pain management, focusing on diagnosing the root cause of your discomfort rather than merely masking symptoms. With a commitment to avoiding opioids and surgeries whenever possible, we offer innovative treatments tailored to your individual needs. Schedule your consultation to start building a strong partnership with board-certified pain doctors committed to your health and well-being.
FEATURED POSTS BY PAIN DOCTORS