Table of contents
Get treated by pain treatment industry leaders
What Is Bursitis? A Comprehensive Medical Overview
Medically verified
Last updated on 03/17/2026

By Dr. George Hanna
Pain Doctor at Pain Treatment Specialists
University of Pennsylvania
Double Certified in Anesthesiology and Pain Medicine.
Understanding what bursitis is requires a look at the protective structures within your joints. For many patients, bursitis is a condition where the essential cushions of the joint—the bursa sacs—become inflamed, leading to localized pain and a significant restriction in mobility.

At Pain Treatment Specialists, we prioritize an academic care model to address the complexities of joint inflammation. By using an evidence-based approach, we help you understand the triggers of your bursitis, allowing us to move toward a precise diagnosis and a non-surgical treatment plan.
The Medical Definition of Bursitis
Bursitis is the inflammation or irritation of a bursa. A bursa is a small, fluid-filled sac that functions as a gliding surface to reduce friction between moving tissues in your body. There are over 150 bursae in the human body, located primarily near major joints like the shoulders, elbows, hips, and knees. In a healthy state, these sacs are thin and produce just enough synovial fluid to allow tendons and muscles to slide smoothly over bone. When a bursa becomes inflamed, it thickens and produces excess fluid, turning a low-friction environment into a source of pain and resistance.
Because bursae are located at critical mechanical junctions, their inflammation can significantly impact joint function. At Pain Treatment Specialists, we define bursitis not just by the localized swelling, but by the functional limitations it places on a patient’s life. By identifying exactly which bursa is involved—whether it is the subacromial bursa in the shoulder or the trochanteric bursa in the hip—we can develop a targeted medical strategy to resolve the inflammation. This precision is essential for distinguishing bursitis from other conditions like arthritis or ligament tears.
What Causes a Bursa to Inflame?
The most common cause of bursitis is repetitive movement or prolonged pressure on a specific joint. Activities like throwing a ball, lifting objects overhead, or even leaning on your elbows for long periods can irritate the bursa. Sudden injuries, such as a fall onto the hip or a direct blow to the knee, can also cause acute traumatic bursitis. Additionally, as we age, the tendons and bursae naturally become less resilient, making older adults more susceptible to chronic inflammation. Systemic conditions like rheumatoid arthritis or gout can also trigger inflammatory responses within these sacs.
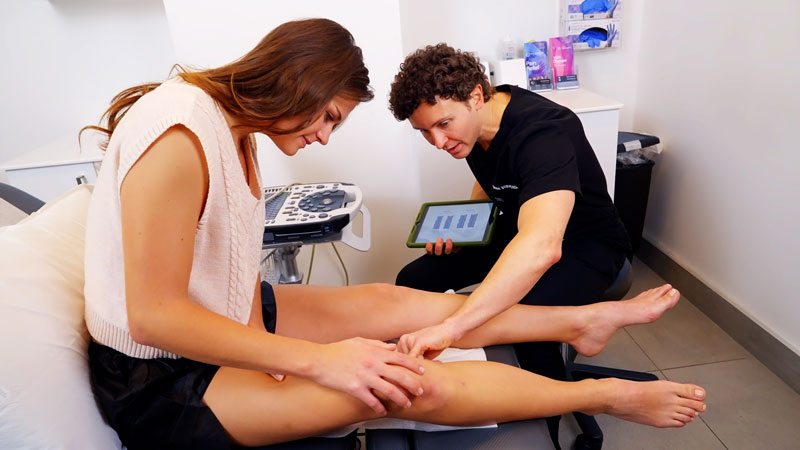
Understanding the “why” behind your bursitis is a core part of our academic approach. If a bursa is chronically inflamed, it is often a sign of an underlying mechanical imbalance, such as poor posture or muscle weakness, that is placing an uneven load on the joint. Our board-certified specialists use advanced diagnostics, including high-resolution ultrasound, to visualize the bursa in real-time. This allows us to see the degree of swelling and fluid accumulation, ensuring that our treatment plan addresses both the immediate pain and the physical stressors that caused the inflammation to begin with.
When Should You See a Specialist for Bursitis?
You should seek a specialist’s evaluation if your joint pain is persistent, recurs frequently, or is accompanied by localized swelling and redness. While mild bursitis may improve with rest, chronic inflammation can lead to a “frozen” joint or secondary muscle strain as you change your movement to avoid pain. If you notice a significant loss in your range of motion—such as difficulty reaching behind your back or walking upstairs—it is a clear indication that the bursa inflammation has reached a clinical threshold that requires specialized interventional care to resolve safely.
A consultation at Pain Treatment Specialists provides the diagnostic clarity needed to move forward with confidence. Our board-certified physicians specialize in non-surgical recovery, offering the same high-level expertise found at top academic medical institutions. We take the time to explain your diagnosis and how interventional techniques—such as ultrasound-guided injections—can resolve your pain without major surgery. If bursitis is stopping you from staying active, a professional diagnostic workup is the most reliable way to start your journey toward a life that is no longer limited by joint inflammation.
Most PPO insurances cover pain treatment!
and 100+ more
Questions about your insurance coverage?
We know health insurance is confusing, fortunately our expert team is always willing to help!
Just call us (877) 461-0819 to verify your coverage or answer any concern you may have.
About the Medical Team at Pain Treatment Specialists

At Pain Treatment Specialists, our approach is rooted in an academic, evidence-based model of care that prioritizes patient safety and long-term outcomes. Our clinicians are trained at the nation’s leading medical institutions, bringing a high level of expertise to the diagnosis and treatment of complex pain conditions.
Clinical leadership at Pain Treatment Specialists is guided by a panel of board-certified specialists responsible for establishing and maintaining the clinic’s medical standards. Their approach reflects training developed at nationally recognized academic institutions such as Harvard, Yale, and Columbia.
All physicians follow a structured, highly standardized clinical model. This includes ongoing training in the latest non-surgical treatments, continuous review of emerging research, and strict adherence to proven safety and quality protocols to ensure consistent results.
If you’re experiencing symptoms and want clarity about the cause, a medical evaluation can help guide the next step. Schedule a Consultation

See how we change lives
Start Your Journey to
Pain-Free Life
At Pain Treatment Specialists, education is considered a core part of treatment. Patients are encouraged to understand their condition, their options, and the reasoning behind each recommendation to foster a collaborative recovery environment.
If you’re experiencing symptoms and want clarity about the cause, a medical evaluation can help guide the next step.
Take control, start feeling better
Take the first step to personalized care for your type of acute and chronic pain. One of our patient coordinators will call you to schedule your visit and verify insurance coverage.